Written by Marijn Overvest | Reviewed by Sjoerd Goedhart | Fact Checked by Ruud Emonds | Our editorial policy
Healthcare Procurement: Definition, Strategies + Examples
What is healthcare procurement?
- The process of sourcing and purchasing goods and services that directly support patient care, from medical devices and pharmaceuticals to cleaning, catering, and digital systems.
- Hospitals and public health organizations achieve better patient outcomes by balancing cost efficiency, quality, and sustainability in every purchasing decision.
- Healthcare procurement ensures transparency, ethics, and long-term resilience by integrating responsible suppliers, digital tools, and value-based strategies into the healthcare supply chain.
What is Healthcare Procurement?
In simple terms, healthcare procurement covers how public and private organizations plan, source, and purchase everything from pharmaceuticals and protective equipment to cleaning services and digital systems. But unlike other industries, procurement decisions here can directly affect human lives.
The main challenge is balancing cost efficiency, clinical effectiveness, and quality of care. Hospitals must stay financially sustainable without compromising patient well-being. As Unite.eu notes, responsible procurement means looking beyond price, evaluating suppliers on ethics, quality, and environmental standards.
This marks a shift toward value-based healthcare, where outcomes matter more than outputs. Procurement teams are expected not just to save costs but to create long-term value by sourcing innovative, sustainable, and patient-centered solutions.
The COVID-19 pandemic made this clearer than ever. Global shortages of ventilators, PPE, and medicines revealed that procurement must be both efficient and agile, able to adapt fast when crises strike.
Integrity and transparency are equally vital. The Transparency International Health Initiative shows that opaque tendering and corruption in healthcare waste billions every year. Open competition and ethical procurement rebuild public trust and ensure that funds truly serve patients.
Finally, sustainability has become central. Hospitals face rising pressure to cut emissions, source responsibly, and integrate circular-economy principles.
Procurement is no longer a backstage operation. It’s a driver of innovation, accountability, and better care, shaping how modern health systems deliver value to every patient.
Procurement Models and Strategies in Healthcare
No two healthcare systems are the same, and neither are their procurement models. Each hospital or ministry must decide how to source critical goods and services while ensuring transparency, accountability, and patient safety. Choosing the right procurement strategy can determine not only operational efficiency but also the level of trust between providers, suppliers, and patients.
Here are the main procurement models shaping healthcare systems today, along with their advantages and challenges.
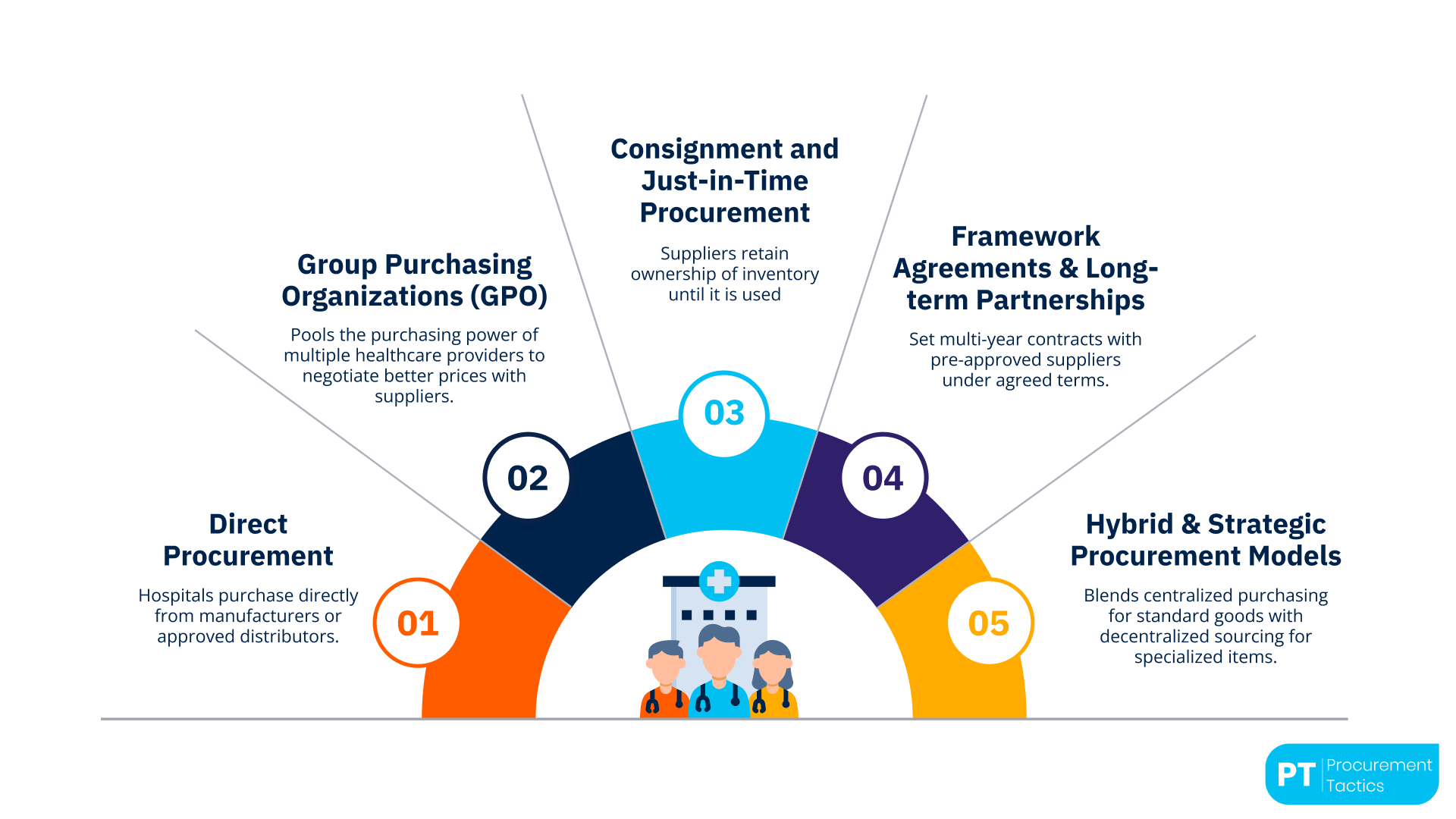
1. Direct Procurement
Direct procurement means hospitals or health agencies buy products and services directly from manufacturers or authorized distributors. This model is common for large hospitals or health systems that have strong internal procurement teams and high purchasing volumes.
Advantages:
- Greater control over supplier selection, quality standards, and delivery schedules.
- Shorter communication lines between buyer and supplier, which reduces the risk of misunderstandings or product mismatches.
- Ability to negotiate directly for better pricing or customized solutions.
Challenges:
- Requires significant procurement expertise and administrative resources.
- Limited economies of scale for smaller hospitals.
- Increased exposure to supply disruptions if only a few vendors are used.
Direct procurement works best when organizations have mature internal systems and want to maintain strict control over product quality and supplier reliability, for instance, in specialized medical equipment or high-risk pharmaceutical categories.
2. Group Purchasing Organizations (GPOs)
Many healthcare institutions, especially smaller ones, join forces through Group Purchasing Organizations (GPOs). These entities aggregate the purchasing power of multiple hospitals or clinics to negotiate better prices and standardized contracts with suppliers.
Advantages:
- Significant cost savings through volume discounts and pre-negotiated contracts.
- Access to a vetted supplier base with proven compliance and quality credentials.
- Reduced administrative burden for member organizations.
Challenges:
- Less flexibility to choose specific products or brands outside of the group framework.
- Risk of over-standardization that may not meet the clinical needs of every facility.
- Dependence on the GPO’s governance and negotiation strength.
GPOs are particularly effective for routine consumables, such as gloves, syringes, or general hospital supplies, where standardization adds efficiency without harming care quality.
However, for highly specialized areas (like oncology drugs or diagnostic technology), a more tailored approach is often needed.
3. Consignment and Just-in-Time Procurement
Some hospitals adopt consignment models, where suppliers retain ownership of inventory until it is used. This approach minimizes storage costs and reduces waste, as unused products can be returned or replaced before expiration. Another related strategy is Just-in-Time (JIT) procurement, where supplies arrive precisely when needed for clinical operations.
Advantages:
- Reduced inventory and storage costs.
- Improved cash flow since payment occurs upon consumption.
- Better coordination with suppliers and reduced product obsolescence.
Challenges:
- High dependence on supply chain reliability.
- Risk of stockouts during sudden demand surges or transport disruptions.
- Requires precise forecasting and seamless communication systems.
During the pandemic, many hospitals discovered both the strengths and weaknesses of JIT models. While they optimized efficiency in stable periods, they struggled under global shocks, highlighting the need for hybrid systems that combine flexibility with safety stock.
4. Framework Agreements and Long-Term Partnerships
Framework agreements allow healthcare institutions to establish multi-year contracts with pre-approved suppliers under defined conditions. These agreements streamline future purchases, avoiding repetitive tendering while maintaining competition among approved vendors.
Advantages:
- Faster procurement cycles.
- Predictable pricing and reliable supplier relationships.
- Easier monitoring of supplier performance over time.
Challenges:
- Initial setup requires detailed evaluation and legal expertise.
- Overreliance on a limited pool of suppliers can reduce flexibility.
- Market changes during long-term contracts may affect pricing fairness.
5. Hybrid and Strategic Procurement Models
Modern healthcare systems increasingly use hybrid procurement, combining centralized purchasing for standard goods and decentralized sourcing for specialized items. This balance allows hospitals to capture economies of scale while preserving clinical flexibility.
Strategic procurement takes this a step further. It integrates procurement goals with overall healthcare strategy, such as improving patient outcomes, enabling innovation, and promoting sustainability.
This approach views procurement as a value creator rather than a cost center.
Strategic healthcare procurement involves:
- Early involvement of clinicians in decision-making.
- Lifecycle cost analysis instead of unit price comparison.
- Evaluation of suppliers based on ESG metrics.
- Continuous supplier performance monitoring.
In this model, success is measured not by how much money is saved, but by how much value is delivered, for both patients and the healthcare system as a whole.
5 Examples of Modern Healthcare Procurement
Healthcare procurement is becoming a cornerstone of patient care, transparency, and sustainability. The following examples from NHS England, Denmark, and Singapore show how health systems around the world are turning procurement into a driver of innovation, resilience, and trust.
1. NHS England: Value-Based and Transparent Procurement
As one of the world’s largest public health systems, the UK’s National Health Service (NHS) manages billions in annual procurement spending. To ensure every pound supports better care, the NHS has pioneered value-based procurement, focusing on outcomes rather than price alone.
What they do:
The NHS redefined procurement as a clinical and ethical function, not merely an administrative one. Its approach integrates patient outcomes, sustainability, and social value into supplier evaluation. The NHS Supply Chain initiative connects more than 200 trusts and 7,000 suppliers through unified contracts that reward innovation and long-term performance instead of short-term savings.
How it works:
Through its NHS Supply Chain program, the NHS introduced digital procurement platforms and transparent tendering processes. Suppliers are scored based on lifecycle costs, environmental performance, and contributions to patient outcomes. The system also tracks product effectiveness and waste reduction through centralized data dashboards.
Why it’s effective:
This model delivers better patient outcomes and reduces procurement costs by focusing on value instead of volume. Transparency mechanisms limit corruption risks, while standardized contracts cut administrative time and improve supplier accountability.
2. Denmark: Green Public Procurement in Hospitals
Denmark leads Europe in sustainable healthcare by embedding climate responsibility into its procurement system. The country recognized that reducing the carbon footprint of hospitals is as crucial as treating patients themselves.
What they do:
Denmark made green public procurement (GPP) a national priority, integrating sustainability into every hospital’s purchasing decision. The Ministry of Health and the Environment Agency jointly developed mandatory environmental criteria for medical equipment, construction, and facility services. Hospitals must now consider lifecycle impacts, from production emissions to disposal, when awarding contracts.
How it works:
Hospitals must apply environmental criteria such as CO₂ reduction, waste minimization, and recyclable packaging when evaluating suppliers. The Ministry of Health collaborates with the Environment Agency to align procurement with national climate targets.
Why it’s effective:
By reducing waste and focusing on circular-economy principles, Denmark’s hospitals lower both emissions and long-term costs. Procurement becomes a tool for climate action, not just a cost-management process.
3. Singapore: Centralized and Data-Driven Procurement
Singapore’s healthcare system faces high population density and limited space, making efficiency and data accuracy vital. Its response has been to create a unified, high-tech procurement network that integrates all public hospitals.
What they do:
Singapore’s Integrated Health Information Systems (IHiS) created a national digital procurement framework that connects all public hospitals, polyclinics, and specialty centers. This system integrates procurement with supply-chain analytics and financial planning, enabling end-to-end visibility from requisition to delivery. The government positions procurement as a strategic enabler of healthcare innovation, not just a back-office process.
How it works:
Procurement is fully digitalized, from supplier registration to contract management. Real-time data on supplier performance and stock levels supports predictive purchasing and eliminates stockouts.
Why it’s effective:
The centralized digital approach reduced procurement lead times, improved transparency, and saved millions through automated analysis. By combining technology and governance, Singapore created one of the most efficient healthcare procurement systems in Asia.
4. United States: Group Purchasing for Scale and Resilience
With a vast and fragmented healthcare system, U.S. hospitals face challenges in cost control and supply chain stability. Group purchasing organizations (GPOs) have become essential in consolidating buying power and ensuring resilience.
What they do:
Leading GPOs such as Vizient and Premier Inc. negotiate on behalf of member hospitals, leveraging collective demand to secure better pricing, compliance, and sustainability outcomes. They also provide analytics services, benchmarking tools, and supplier-risk monitoring. Some GPOs have evolved into full strategic-sourcing partners, advising hospitals on cost optimization and product innovation.
How it works:
Hospitals join networks that consolidate demand and use data analytics to evaluate supplier performance and pricing trends. After COVID-19, GPOs also began building regional inventories and diversifying supplier bases to prevent future disruptions.
Why it’s effective:
The GPO model achieves cost savings of up to 30%, ensures product quality through supplier vetting, and strengthens the resilience of healthcare supply chains during crises.
5. WHO and Global South Initiatives: Transparent Procurement for Access
In low- and middle-income countries, weak oversight and paper-based procurement often lead to corruption and medicine shortages. The World Health Organization (WHO) and Global Fund are helping governments modernize through transparency and digital reform.
What they do:
The WHO’s Good Governance for Medicines program and the Global Fund’s Procurement and Supply Management Framework help countries establish fair, competitive, and digital procurement systems. These initiatives strengthen national agencies’ ability to plan tenders, negotiate ethically, and monitor suppliers. The goal is to ensure that every public dollar spent on health contributes to real patient outcomes.
How it works:
Countries such as Kenya and Ghana implemented open contracting platforms to publish tenders, track supplier performance, and ensure fair competition.
Why it’s effective:
These systems reduced medicine stockouts by nearly 40%, cut procurement costs, and increased public confidence. Transparency helped redirect funds toward essential drugs and improve health equity.
Key Challenges and Solutions in Healthcare Procurement
Procurement in healthcare operates under extraordinary pressure. Every purchase must meet strict legal, ethical, and medical standards, all while keeping costs under control and ensuring patient safety. Yet, despite its critical importance, healthcare procurement still faces multiple barriers that slow progress, limit transparency, and weaken resilience.
Here are the main challenges and the solutions emerging across modern healthcare systems.
Healthcare procurement faces a unique mix of regulatory, ethical, and operational challenges. But each challenge carries its own solution, one rooted in strategy, transparency, and collaboration.
The future of healthcare procurement depends on aligning efficiency with responsibility, innovation with integrity, and cost with care. Those that achieve this balance will not only deliver savings but also transform patient care and trust in public health systems.
Conclusion
Healthcare procurement is no longer just a support function; it is the backbone of modern healthcare delivery. By combining ethics, transparency, sustainability, and data-driven strategy, procurement professionals directly influence how efficiently hospitals operate and how safely patients receive care.
Across the world, organizations are rethinking procurement not as a cost center but as a strategic enabler of better outcomes. From the NHS’s value-based sourcing to Singapore’s predictive analytics and Denmark’s green procurement policies, every example proves that procurement decisions shape lives.
The path forward is clear: healthcare procurement must stay transparent, technologically adaptive, and aligned with sustainability and clinical priorities. The systems that achieve this balance will not only save money, but they will also save lives and rebuild public trust in healthcare.
Frequentlyasked questions
What is healthcare procurement?
Healthcare procurement is the process of sourcing and purchasing goods and services that directly support patient care, including medical devices, pharmaceuticals, catering, and digital systems.
Why is healthcare procurement important?
Effective procurement helps hospitals balance cost efficiency, service quality, and patient outcomes, while minimizing waste and corruption. In short, good procurement means better care, safer hospitals, and more efficient use of public resources.
What are the main types of healthcare procurement?
The main models include direct procurement, where hospitals buy directly from suppliers; group purchasing, where several institutions combine demand for better pricing; framework agreements for long-term supplier partnerships; and centralized procurement, where national or regional authorities manage sourcing to ensure consistency and transparency.
About the author
My name is Marijn Overvest, I’m the founder of Procurement Tactics. I have a deep passion for procurement, and I’ve upskilled over 200 procurement teams from all over the world. When I’m not working, I love running and cycling.

Procurement Roles Overview
Click on a role to learn more




